Prostate Cancer Susceptibility Appears Different for Different Races
Prostate cancer is among the most genetically influenced cancers. Out of the millions of possible SNPs that exist in the human genome; so far, approximately 40 have been associated with prostate cancer risk, and this study looked at 36 of those.
Previous studies have established differences in prostate cancer incidence rates among different ethnic groups. For example, in the U.S., the incidence rate per 100,000 population is 231 in African Americans, 143 in Caucasians, 127 in Hispanics and 80 in Asians.
Baseline Differences
Genetic fingerprints representing the frequencies of the 36 prostate cancer risk alleles among three races.:
The pink line is for African Americans; the blue line is for Caucasians; and the yellow one is for Hispanics.
The patterns of three lines are different: 34 out of 36 SNPs are significantly different in the allele frequencies based upon race, with the exception of 2 SNPs on chromosome 8q24.
African American men had the highest frequencies for about 45% of these SNPs. Caucasian men had the highest frequencies for about 30% of these SNPs. For the other 25% of these SNPs, Hispanic men had the highest frequencies.
The goal of this study was to determine the relative baseline differences in the frequency of prostate cancer susceptibility alleles in healthy men of difference ethnic groups.
Two thousand healthy volunteers were included in the study and genotyped for 36 prostate cancer risk SNPs.
African Americans were carriers of significantly higher average number of total risk alleles compared to Caucasian and Hispanic men. These rates correspond roughly with the incidence rates of prostate cancer in the U.S. population.
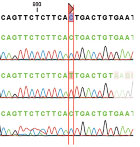
SNP is a change (a variant) in which a single base in the DNA differs from the usual base at that position. It occurs when a single nucleotide (building block of DNA) is replaced with another. It can be thought of as the location of the change.
Allele: is one of the altered forms of any segment of a chromosome. It can be thought of as the actual code or letter change.
Researchers look at specific DNA codes of known genes and variations within these genes called alleles.
Most people have seen the very long and involved list of alphabet letters that represent a genetic code. In one area a part of a code might be CCAT but in a substantial number of men with prostate cancer, that code area is CAAT.
The place where the changed code is spotted is the SNP and, in the example above, in the second letter: C to A) is the allele variation.
Because the majority of genetic studies that established risk alleles are performed in white men, there are almost certainly many other risk SNPs that are found in African Americans, Hispanics and Asians that have not bee tested in our studies.
Conclusion
The frequencies of prostate cancer risk alleles differ by ethnic groups, and these differences probably account for some of the differences in prostate cancer incidence rates in the U.S. population.
AUA Poster Presentation: Prostate Cancer Risk Alleles Are Present at Significantly Different Frequency in Healthy Volunteers of Different Races: Qiaoyan Hu; Brian T. Helfand, MD, PhD; Stacy Loeb, MD; Nikola A. Baumann, MD; William J. Catalona, MD
AUA Poster Presentation: Prostate Cancer Risk Alleles Are Present at Significantly Different Frequency in Healthy Volunteers of Different Races











