How Long Can Surgery Be Safely Delayed In Men With Low Risk Prostate Cancer?

Men with low-risk prostate cancer (CaP) have multiple options for treatment including radical prostatectomy (RP), radiation therapy and active surveillance.
Increased acceptance of surveillance, scheduling issues, time spent on researching various options, and other circumstances may lead to extended time from biopsy to surgery.
This study* presented at a recent AUA meeting addresses a question created by these treatment alternatives: How long can surgery be safely delayed in men with low risk prostate cancer?
Previous data on surgical delay in low-risk prostate cancer is scant and controversial.
The aim of this study was to determine the impact of delaying radical prostatectomy on recurrence rates in a population diagnosed with seemingly low-risk prostate cancer (Gleason sum of 6 or less, normal prostate on digital rectal examination, and PSA less than 10 ng/ml).
The study group included 1,111 men (Catalona) who underwent radical prostatectomy. Pathologic tumor features and recurrence rates were compared in men operated on within six months of diagnosis versus those operated on six months or more following diagnosis.
In some areas, the time span made no significant difference: proportion of organ-confined disease, extra-capsular extension, positive surgical margins, seminal vesicle extension, or lymphnode metastases.
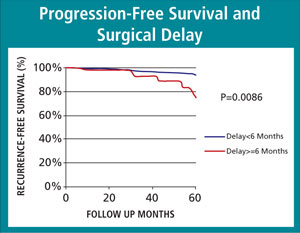
However, in two important areas, the delay did show a statistical effect.
A surgical delay of six months or more
- was associated with a significantly greater proportion of Gleason score 7 to 10 tumors on final pathology examination of the prostate specimen and
- was associated with more than double the frequency of cancer recurrence. (Specifically, the recurrence rate was 5% in men with early radical prostatectomy compared to 12% of those treated at or beyond six months of diagnosis.)
The study concludes: A delay in having a radical prostatectomy for 6 months or longer after diagnosis shows a statistically significant adverse association in outcomes, specifically more high-grade disease and more recurrence.
Low-risk patients should be counseled about the possibility of worse outcomes with a delay in surgical treatment.
Further studies are necessary to investigate whether these findings will translate into a difference in prostate cancer mortality rates.
* How Long Can Surgery Be Safely Delayed In Men With Low Risk Prostate Cancer? Gustavo F. Carvalhal, MD; Stacy Loeb, MD; Donghui Kan; Matthias D. Hofer, MD, PhD; Jessica T. Casey, MD; Brian T. Helfand, MD, PhD; Daniel O’Brien; William J. Catalona, MD Supported in part of the Urological Research Foundation, Prostate SPORE grant and the Robert H. Lurie Comprehensive Cancer Center grant.
How Long Can Surgery Be Safely Delayed In Men With Low Risk Prostate Cancer?











