PSA Velocity Risk Count Helps Identify Clinically Significant Prostate Cancer

(This article is prepared for QUEST readers from a study* presented at a recent AUA meeting.)

Despite considerable refinement in radical prostatectomy and radiation therapy over the past few decades, all treatments for prostate cancer proceed as if a patient’s disease is potentially life threatening.
Low-risk prostate cancer is simply not reliably identifiable at the time of diagnosis from existing information and, at times, cancers having PSA values below the biopsy threshold can be significant.
A specific measurement for PSA Velocity, called PSAV risk count, could possibly assist in identifying which are threatening prostate cancers or tumors that need to be identified and treated.
Risk count is designed to find the aggressive tumors.
Threatening or Non-Threatening CaP
PSAV risk count could possibly assist in identifying threatening prostate cancer or tumors that might not cause symptoms.
PSA Velocity (PSAV) is the rate of increase of PSA in an individual over time. PSAV, the change in PSA per year, has become an important tool for detecting prostate cancer early, for distinguishing prostate cancer from benign conditions, and for assisting in interpretations of PSA results.
How that rate of PSA increase relates to PSA values in general and to predictions for aggressive prostate cancers in specific was the focus of this study.
Specifically, this study examined whether PSAV risk count could increase the accuracy of screening for overall and for potentially life-threatening prostate cancers.
Risk Count of 2
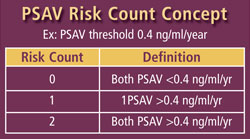
Risk count means that for men with at least 2 years of serial PSA screening, the PSAV is calculated 2 years in a row to see if one, both or neither are above the critical threshold value of .4 ng/ml/year.
For example, a PSA velocity greater than approximately 0.4 ng/ml/year has previously been shown to predict life-threatening prostate cancer. If a man has 2 serial PSAV measurements, did one, both, or neither exceed 0.4 ng/ml/year?
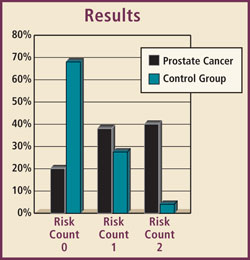
What the study found is that in 40% of CaP patients (Catalona), the PSAV twice exceeded 0.4 ng/ml in a year, (a risk count of 2); whereas that risk count was only 4% in men without prostate cancer.
In addition, after adjusting for age and PSA, the study found a PSAV risk count of 2 was associated with more than 8 times increased risk of prostate cancer and more than 5 times increased risk of high-grade (Gleason score 8 to 10) on biopsy.
Compared to information that used only age and total PSA, the addition of PSAV risk count significantly added to diagnostic accuracy and identified more patients with respect to their risk of high-grade cancer.
Serial PSA History
The study showed that sustained rises in PSA are suggestive of a significantly greater risk of prostate cancer, particularly high-grade cancer.
Compared to PSA alone, PSAV risk count may be useful for reducing unnecessary biopsies and diagnoses of low-risk CaP. The findings suggest that a prostate biopsy trigger based on the PSA risk count might reduce the number of unnecessary prostate biopsies, the diagnosis of low grade, indolent cancer, and correspondingly, the overtreatment of these cancers.
PSA risk count is only feasible with men who have a serial PSA history, but many men present with a lengthy PSA history of prior values. PSA risk count makes a baseline PSA and annual PSA testing two essential practices. When the PSA history is available, this study shows that risk count has a robust association with prostate cancer risk, and especially high-grade disease.
Also, risk count can sound alarms that might otherwise go unheeded. For example, if someone has a PSA of 0.4 and it goes up to 0.8, that’s still so low that most urologists wouldn’t biopsy, even if it went up again to 1.4.
Those numbers are still below the biopsy threshold but the risk count is 2 so that patient is at much greater risk of having significant disease.
In this way, risk count may act as an early warning sign for potentially life-threatening prostate cancer even while PSA is still low.
Future studies are recommended to evaluate the use of PSAV risk count as an indication for prostate biopsy.
* PSA Velocity Risk Count Helps Identify Clinically Significant Prostate Cancer Stacy Loeb, MD; H. Ballentine Carter, MD; E. Jeffrey Metter, MD; Donghui Kan, Kimberly A. Roehl, and William J. Catalona, MD
(Catalona)










