Underdiagnosis and Overdiagnosis of Prostate Cancer
(Prepared by Cecilia Lacks, PhD, from AUA presentation by William J. Catalona, MD and his Research Collaborators) INTRO: In 2005, prostate cancer accounted for approximately one third of new cancer diagnoses in men in the United States.
 Some men with clinically localized cancer undergo radical prostatectomy, but the final pathology report shows more extensive cancer.
Some men with clinically localized cancer undergo radical prostatectomy, but the final pathology report shows more extensive cancer.
Conversely, some in the medical field are concerned that widespread screening has led to the diagnosis and treatment of cancers that may never have caused medical problems if left untreated or undiagnosed.
QUESTION: Is a patient more likely to be “underdiagnosed” or “overdiagnosed” in the PSA era (basically the last 15 years).
STUDY: 3,331 men were treated by radical prostatectomy during two times periods: 1989-95 when the PSA cutoff for biopsy was 4.0 and after 1995 when the recommended PSA cutoff for biopsy was 2.5.
We examined the percentage of men who met the criteria for “overdiagnosed” and “underdiagnosed” prostate cancer.
We defined overdiagnosis using the published criteria (Ohori) which includes a cancer volume less than 0.5cc’s, organ-confined, and no Gleason pattern of 4 or 5. (Note: It is impossible to predict that an individual cancer is insignificant in any given patient, particularly a young patient, because tumors can develop mutations and become more aggressive over time.)
We defined underdiagnosis using criteria (Catalona) which includes men who were found at radical prostatectomy to have advanced pathological features including: tumor outside the prostate, positive surgical margins, or lymph node metastases.
Using the 4ng/ml cutoff, 1.3 percent of men were treated for possible overdiagnosed tumors and 30 percent met the criteria for underdiagnosis.
Using the 2.5 ng/ml cutoff, the rates were 7.1 percent overdiagnosed and 26 percent underdiagnosed.
Clearly, far more men were underdiagnosed than overdiagnosed in both eras.
Five year progression-free survival rates for men who were underdiagnosed was 79%, which was, as expected, 13 percentage points lower than those men who were not underdiagnosed.
Lowering the PSA threshold from 4ng/mL to 2 resulted in an overall 4 percentage point decrease in the rate of underdiagnosis and a corresponding 7 percentage point increase in five year progression-free survival.
There were some limitations to the study. Tumor volume information was not available for all participants. The definitions of overdiagnosis and underdiagnosis have been challenged by others, and it would be impossible to predict outcomes for these men had they not undergone radical prostatectomy.
CONCLUSION: In this study, more than one-quarter of men were “underdiagnosed,” in that the disease was found to be more advanced in the final pathology report that in the diagnosis and detection process.
At the same time fewer than 8% of men underwent treatment for what has been described as “overdiagnosed.”
Younger men were more likely to be in this 8%, but these men have the longest life expectancy and the most to gain from successful treatment.
Based on the pathology criteria of this study, a patient is significantly more likely to be “underdiagnosed” than “overdiagnosed” in the PSA era.
Theresa Graif, Xiaoying Yu, Chicago, IL; Stacy Loeb, Washington, DC; Sara N. Gashti, Christopher Griffin, Misop Han, Chicago, IL; Kimberly A Roehl, Brian K Suarez, Saint Louis, MO; William J. Catalona, Chicago, IL
Prostate Cancer Vocabulary in the News:
“ Overdiagnosed” and “Underdiagnosed”
The topic of prostate cancer detection is in the news.
And with the coverage is the repeated use of a particular vocabulary describing prostate cancer at diagnosis: overdiagnosed (unimportant* or clinically insignificant**) or underdiagnosed.***
Medical professionals who describe prostate cancer as overdiagnosed if the detections of the cancers would not cause symptoms or death. 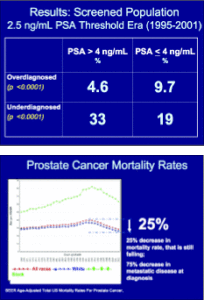
They say the “overtreatment” could have the possibility of unnecessary treatment-related deaths.
If upon biopsy, the cancer is labeled “clinically insignificant,” then some medical professions recommend “watchful waiting,” which means watching for any changes that would indicate the cancer needs to be treated.
“ Underdiagnosed” is the failure to detect prostate cancer at an organ-confined stage with clear surgical margins.
Dr. Catalona is concerned that the great majority of prostate cancers present in a quantity to register in PSA testing and confirmed in biopsy should be treated as soon as possible after diagnosis.
He is even more concerned with prostate cancer that is underdiagnosed.
*unimportant (Ohori criteria) when the tumors have a volume equal to or less than 0.5cm3, are confined to the prostate, and have a Gleason score of less than 7.
**insignificant (Epstein criteria) ) when the tumors have a volume equal to or less than 0.2cm3, are confined to the prostate, and have a Gleason score of less than 7.
***underdiagnosed (Catalona criteria) when the tumors are non- prostate organ confined meaning one or more of the following: pathology (examining prostate after it’s been removed) stage T3 or greater, positive surgical margins, lymph node metastases, or extracapsular tumor extension.










