Test Results and What Should Be Done About Them
(Dr. Catalona received the 2005 Huggins Award from the Society of Urologic Oncology and gave the Award Lecture on The PSA Dilemma in the Overdiagnosis and Underdiagnosis of Prostate Cancer. This article in QUEST is a summary of that lecture and ensuing interviews with QUEST readers in mind.)
overdiagnosing in young men is impossible to prove
 The goal of prostate cancer screening is to reduce prostate cancer-related suffering through early detection of curable cancers that can cause disability or death.
The goal of prostate cancer screening is to reduce prostate cancer-related suffering through early detection of curable cancers that can cause disability or death.
At the same time, the goal is to minimize unnecessary diagnosis, and therefore unnecessary treatment-related side effects and deaths.
The strategy is to avoid overdiagnosis and overtreatment of harmless cancers and also to avoid underdiagnosis and undertreatment of harmful cancers.
The ultimate goal is to ensure high-quality care for all treated patients.
The PSA dilemma is how to use PSA to diagnose prostate cancer early enough to avoid underdiagnosis, but not too early to avoid overdiagnosis?
The concern is more than statistical, but figures are important in a discussion of over and underdiagnosis.
In the United States States it is estimated that in the year 2006, 234,460 new cases of prostate cancer will be diagnosed (33% of the new cancer cases in men) and 27,350 prostate cancers deaths will occur (9% of cancer deaths in men).
The lifetime risk for a US man being diagnosed with prostate cancer is 18%, and 3.1% of all men in the US will die from prostate cancer. Clearly, prostate cancer affects a good many men.
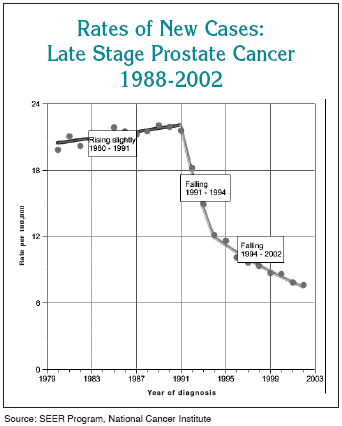
PSA testing has resulted in a decreased incidence of metastatic disease at the time of diagnosis by 75% and a decreased death rate of 25%.
In countries that practice CaP screening, mortality due to CaP has decreased since 1992, as compared to increases during the same time period in countries that do not practice screening.
The ratio of CaP diagnosis to CaP death is 8:1 in the US as compared to 2:1 in countries that do not screen.
People who argue that some CaP is overdiagnosed define it as diagnosing and treating cancers that would not cause symptoms or death.
Statistics counter the argument of overdiagnosis: 30% of patients are “underdiagnosed” (i.e., diagnosed after the cancer has spread to the margin of the prostate gland or beyond). In a young patient this situation is a frightening one.
In a personal review of Dr. Catalona’s last 200 patients,12.5% of cancers were found on the pradical prostatectomy specimen to be organ confined, Gleason grade of 6 or less, and a volume of less than 0.5cc.
Dr. Catalona does not consider these tumors to be insignificant cancer because, with time, tumors mutate and become more aggressive, and these changes are not predictable.
 Removing a prostate with so-called ” insignificant” cancers can also mean a life-threatening change was eliminated before it happened. Overdiagnosing in young men is impossible to prove because small, undistinguished tumors can acquire aggressive features over time.
Removing a prostate with so-called ” insignificant” cancers can also mean a life-threatening change was eliminated before it happened. Overdiagnosing in young men is impossible to prove because small, undistinguished tumors can acquire aggressive features over time.
Other factors are important in evaluating what a PSA score means, but, clearly, PSA is a critical element in diagnosing prostate cancer. Total PSA correlates with risk of prostate cancer, PSA velocity and mortality.
Using additional information makes the PSA test results more effective. For example, PSA density is an underutilized tool in diagnosing CaP.
Also, a more conservative PSA velocity cutoff of 0.4ng/ml/year would be more accurate than the existing cutoff of 0.75 ng/ml/year for recommending a biopsy in men whose total PSA level is less than 4.0 ng/ml..
Measuring the percentage of freePSA and complexed PSA is helpful in interpreting PSA results. The lower the percentage of free PSA (less than 15%), the more likely cancer is present.
And in the future, proPSA (an isoform of PSA) might be used to more effectively interpret PSA results.
At present, PSA provides a useful basis for risk assessment across all PSA levels.
It is not widely appreciated that the median PSA value in men in their 40s and 50s who do not have prostate cancer is less than 1 ng/ml. Even in men older than 60 years without known prostate cancer, the median PSA value is less than 1.5 ng/ml.
So, if a man has a PSA value higher than these levels, it does not absolutely mean that he has cancer, but it does mean that he is at a substantially higher risk.The total PSA value is a powerful marker for prostate cancer.
Appropriate use of PSA based techniques is valuable in minimizing underdiagnosis and overdiagnosis of CaP.
A Patient’s Perspective:
Men don’t live in a space called “overtreatment/undertreatment.”
We live in the real world.
During our lifetimes, some of us are diagnosed with prostate cancer.
At that point we can choose to be treated or to deny that the cancer will cause us harm: “Let’s wait and see.”
It is, however, only after our lives are over that someone can look back and say, “He made a wise decision.” or “Wasn’t he foolish for not solving the problem when he could have?”
We can only make decisions as best we can at the time when we have to decide. We can’t know the future.
Calculating overtreatment/undertreatment is a nice activity for statisticians, but it doesn’t help a man in the ordinary process of living.
by Jules Reichel, patient and QUEST columnist
Intelligent Use of PSA:
- considers that PSA provides a continuum of risk assessment across all PSA levels
- does not focus only on total PSA cutoff
- repeats PSA measurements, checks for use of different laboratories and rules out prostatitis (infection in the prostate)
- uses PSA density, PSA velocity or doubling time, and % free and % complexed PSA in interpreting PSA results
- avoids underdiagnosis by screening early and frequently and by identifying most aggressive cancers by PSA velocity and other PSA derivatives and isoforms.











