Drop in Prostate Cancer Mortality Rates During PSA Screening Era
At the end of 2008, the National Cancer Institute published its findings on the incidence of various cancers and cancer-caused deaths with encouraging news regarding most cancers and especially for prostate cancer.
The media picked up the drop in incidence of cancer, the first time ever. Dr. Catalona thought the big news was something else for prostate cancer.
“Since 1992 (the year after publication of my paper showing that PSA could be used as a first-line screening test for prostate cancer), rates of death from prostate cancer have fallen 37% in the US, more than for any other cancer in men or women,” he said.
Dr. Catalona noted that while the prostate cancer deaths are down significantly, there is now a decrease in screening which has resulted in a decreased incidence rate of prostate cancer.
“I think the reason for this finding of decreased incidence is that there is less PSA screening due in part to recent anti-screening propaganda. 52% of men 50 or older reported having a PSA test in 2004, down from 58 percent in 2001,” he said.
He finds this decrease in prostate cancer screening alarming because he sees the decrease in deaths from prostate cancer clearly connected to early detection from PSA and DRE screening. More incidence, more early detection, could mean more lowering of death rates from prostate cancer.
The NCI reported the following data on prostate cancer death rates by years:
1975 -1987, an annual increase of 0.9%
1987-1991, an annual increase of 3.0%
In 1991, Dr. Catalona first reported in the New England Journal of Medicine that the PSA test could be used as a first-line screening test for prostate cancer.
1991-1994, an annual decrease of 0.6%
In 1994, Dr. Catalona reported on the pivotal multi-institutional study that led to the approval of PSA as an aid to the early detection of prostate cancer with a 4 ng/ml threshold recommendation for prostate biopsy.
1994-2005, an annual decrease of 4.1%
The figures by ethnic group are different. African-Americans have a 50% higher incidence rate and nearly 200% higher death rate from prostate cancer.
Recent genetic studies, including those performed by Dr. Catalona’s research group, suggest that African-American men are at a higher risk for prostate cancer and for more aggressive prostate cancer because they carry more genetic risk variants in their DNA. African-Americans also are less inclined to participate in annual PSA testing.
“For these men, PSA testing is even more important. So many more lives could be saved with early detection,” Dr. Catalona said.
In an Opinion Piece Dr. Catalona wrote for the Washington Post (August 2008), he explained why the mortality figures are so much more important than the incidence ones:
In the United States, the rate of advanced cancer at the time of diagnosis has fallen 75% since the PSA screening era began, more than for any other cancer. Age-adjusted prostate cancer death rates have declined 37% percent. Statistical studies suggest that 45-70 percent of this decrease is due to PSA screening.
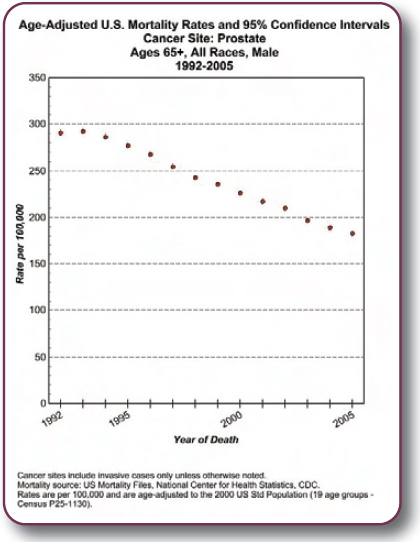
Evidence from U.S. cancer registries shows less advanced cancer and lower prostate cancer death rates in regions where PSA testing is more prevalent.
On a global scale, prostate cancer death rates have decreased in countries where PSA screening and active treatment are typically practiced and have remained stable or increased in countries where screening and active treatment are not practiced.
“PSA tests are a powerful marker for the risk of developing prostate cancer and dying from it. Reports of over-diagnosis and over-treatment are exaggerated. More often, prostate cancer is diagnosed too late rather than too early.
“If screening detected only harmless cancers, treating them could not produce the striking decline in prostate cancer death rates that has occurred,” Dr. Catalona said.
A landmark 2005 study from Canada (Kopec &Goel) showed a significant benefit to early prostate cancer screening that indicated effective screening can prevent as many as 35% less deaths.
“A 35% difference is quite a large amount so from our perspective, it is quite a significant link in the chain supporting that early prostate cancer screening has a positive impact,” Jacek Kopec, study author, said
Otis W. Brawley, MD and chief medical officer of the American Cancer Society, introduced the NCI report by saying, “The drop in incidence seen in this year’s Annual Report is something we’ve been waiting to see for a long time…the continuing drop in mortality is evidence once again of real progress made against cancer, reflecting real gains in prevention, early detection, and treatment,”
In the case of prostate cancer, the drop in incidence and the drop in mortality most likely do not go hand in hand.
The NCI report suggests, “The leveling off of PSA screening may be contributing to the recent decline in prostate cancer incidence because of decreased detection, or reduced number of undiagnosed prevalent cancers.”
“Considering the decrease in mortality rates in the PSA testing era, this leveling off of PSA screening is not necessarily a good direction or good news,” Dr. Catalona said.











